ORIGINAL RESEARCH | https://doi.org/10.5005/jp-journals-10071-23527 |
Not Touching the Face is Harder Than It Sounds: Need for an Intervention
1,3Department of Emergency and Critical Care, Manian Medical Centre, Erode, Tamil Nadu, India
2Department of Dentistry, Manian Medical Centre, Erode, Tamil Nadu, India
4Department of Internal Medicine, Trichy SRM Medical College Hospital and Research Centre, Irungalur, Trichy, Tamil Nadu, India
Corresponding Author: Subramanian Senthilkumaran, Department of Emergency and Critical Care, Manian Medical Centre, Erode, Tamil Nadu, India, Phone: +91 9994634444, e-mail: maniansenthil@yahoo.co.in
How to cite this article Senthilkumaran S, Arathisenthil SV, Meenakshisundaram R, Thirumalaikolundusubramanian P. Not Touching the Face is Harder Than It Sounds: Need for an Intervention. Indian J Crit Care Med 2020;24(8):662–663.
Source of support: Nil
Conflict of interest: None
ABSTRACT
In the novel coronavirus (COVID-19) pandemic, preventive medicine has taken center stage, as there is no vaccine or specific antiviral drug regime used to treat patients. Public health authorities and governments are recommending the practice of social distancing and hand hygiene. Hands are a common vector for the transmission of infection, and frequent face touching is extremely common among the public. We developed and applied a new method to prevent face touching which is of utmost importance to break its cycle and subsequent inoculation of the virus through mucous membranes, thus reducing the risk of transmission of COVID-19.
Keywords: COVID-19, Infection control practices, Prevention.
Face touching is an instinct behavior and helps to overcome stress, regulate emotions, and stimulate memory.1 Interestingly, we share this instinct with monkeys, and it still remains in our memory and resists change.2 Moreover, this behavior was observed among medicos who touch their eyes, nose, or mouth from 23 to 45 times an hour.3 Another study among intensive care nurses revealed that these nurses touched their faces around 5 times an hour4 while on work. Having known this instinct behavior and its contribution to transmission of infections, this has to be curtailed both among healthcare professionals and public through teaching and training for effective infection control.
In the fight against the novel coronavirus, health professionals and the public are being taught and trained continuously on the preventive measures through various audiovisual means. If one continues this instinct behavior, the virus enters the body easily. So, the World Health Organization (WHO) advises on hand washing, cough etiquette, and warns avoidance of (face) touching the eyes, nose, and mouth as an effective means of halting the spread of diseases.5
Telling people “not to touch the face” is easy, but it is harder than it sounds. The problem is “old habits die hard”. Hence, to avoid touching face or different parts of the face, various methods like habit reversal training, substitute behaviors, and social reinforcement were proposed.6 As these do not work well, physical barriers are required.
The physical barriers like wearing a face mask or woolly gloves though prevent from face touching, the gloves may harbor the viruses and other germs too. Usage of artificial intelligence for avoidance of touching face via a webcam7 was attempted, as it recognizes the behavior patterns and sounds a warning if their hand strays to face. Since this has technical constrains, it could not be introduced in the busiest and overcrowded emergency room, thereby necessitating an alternative.
A simple manual method for the healthcare staff is suggested to prevent both unintentional and intentional face touching. The dominant side elbow is taped on the extensor aspect (posteriorly) with an adhesive, non-stretch, hypoallergenic tape of 15–18 cm long on either side of olecranon while keeping the limb in anatomical position. Another tape is applied around the middle of upper arm and a third around the forearm individually winding around the previous tape kept in position as shown in Figure 1. Care shall be taken to shave the upper arm, elbow, and fore arm regions well before taping so as to prevent skin irritation and pain during removal. This manual method allows elbow flexion freely up to 90° without much inconvenience while on work. With the tape in position, if one attempts to bend elbow above 90°, she or he will experience a gentle discomfort which gets aggravated if elbow becomes more and more acute. Overall, the presence of tape by itself and the discomfort experienced likely hinder unintentional and intentional face touching.
We made a humble attempt to find out the usefulness and acceptance of this manual method was applied to nine of our healthcare staff including doctors (three in each shift) after a written informed consent daily before the beginning of work for 6 days. Their elbow movements while on work was monitored via closed-circuit television cameras by two volunteers in each shift. The staff found it beneficial but experienced a sense of something sticking in their dominant upper limb on first two days only. After that they got acclimatized for the manual method. Although in the initial three days, there was no face touching among those on duty, unintentional face touching was observed on two to three occasion among three of a total of nine staff. These small observations clearly indicate that the manual method is likely bring down face touching among healthcare staff while handling patients.
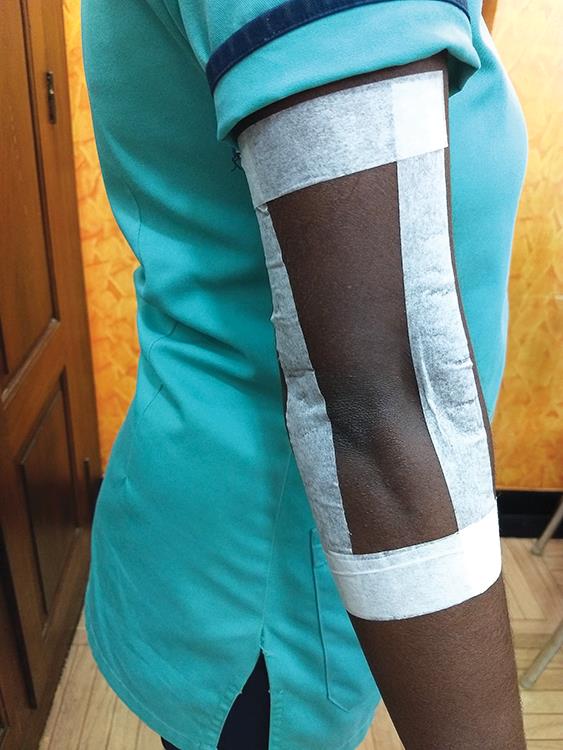
Fig. 1: Manual method with tape in position
Our hands are responsible for the spread of more than 80% of infectious diseases from the common cold and flu to the life-threatening COVID-19 and many others. In view of that, medical and para-medical persons are regularly taught on hand hygiene and reinforced while on work. Despite that, we fail to achieve what we need and want, as habits die hard. With the arrival of COVID-19, we are compelled to change our habits and sustain the habits in our daily practice at hospital, home, and elsewhere. To make it this possible, we have implemented a multifaceted, customized, realistic improvement plan, such as using external cues, Hawthorne effect, electronic monitoring systems and measuring the progress with relevant clinical quality metrics and incentives to positive deviants in the target group. We believe that COVID-19 fear will also make a positive change in all”.
Healthcare staff if accept/agree, this manual method may be attempted for avoidance of “face touching”, till we establish a robust or sophisticated and convenient method. Moreover, large studies are required to accept or refute this simple, affordable, and feasible manual method. The need of the hour is an exclusive curriculum to teach and train health science students on various components (clinical, microbiological, behavioral, and prevention) of “face touching” using different educational methods and be assessed on their cognitive, psychomotor and affective domains, in order to overcome this instinct behavior. Early exposure on avoidance of face touching will likely be remembered and practiced by them in their professional career, which in turn contribute to infection control.
REFERENCES
1. Mueller SM, Martin S, Grunwald M. Self-touch: contact durations and point of touch of spontaneous facial self-touches differ depending on cognitive and emotional load. PLoS One 2019;14(3): e0213677. DOI: 10.1371/journal.pone.0213677.
2. Dimond S, Harries R. Face touching in monkeys, apes and man evolutionary origins and cerebral asymmetry. Neuropsychologia 1984;22(2):227–233. DOI: 10.1016/0028-3932(84)90065-4.
3. Kwok YL, Gralton J, McLaws ML. Face touching: a frequent habit that has implications for hand hygiene. Am J Infect Contr 2015;43(2):112–114. DOI: 10.1016/j.ajic.2014.10.015.
4. Clack L, Scotoni M, Wolfensberger A, Sax H. “First-person view” of pathogen transmission and hand hygiene – use of a new head-mounted video capture and coding tool. Antimicrob Resist Infect Control 2017;6:108. DOI: 10.1186/s13756-017-0267-z.
5. WHO Coronavirus Disease 2019 (COVID-19). WHO, 2020 ((Situation Report 23).)
6. Gollwitzer PM. Implementation intentions: strong effects of simple plans. Am Psychol 1999;54(7):493–503. DOI: 10.1037/0003-066X.54.7.493.
7. Do Not Touch Your Face https://donottouchyourface.com(accessed on 11/04/2020).
________________________
© The Author(s). 2020 Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (https://creativecommons.org/licenses/by-nc/4.0/), which permits unrestricted use, distribution, and non-commercial reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated.