CASE REPORT |
https://doi.org/10.5005/jp-journals-10071-23859 |
A Child with Unilateral Pulmonary Edema due to Mitral Valve Rupture Following Blunt Trauma
1Department of Pediatric Intensive Care, Great Ormond Street Hospital, London, UK.
2-4Department of Pediatric Intensive Care, Kanchi Kamakoti CHILDS Trust Hospital, Chennai, Tamil Nadu, India
Corresponding Author: Satarupa Mukherjee, Department of PICU, Great Ormond Street Hospital, London, UK. Phone: +91 9789877851, e-mail: satarupamukherjee2003@gmail.com
How to cite this article: Mukherjee S, Ravikumar K, Kapalavai SK, Ramachandran B. A Child with Unilateral Pulmonary Edema due to Mitral Valve Rupture Following Blunt Trauma. Indian J Crit Care Med 2021; 25(6):729–731.
Source of support: Nil
Conflict of interest: None
ABSTRACT
A 7-year-old boy was admitted with a history of cough and tachypnea for 1 day. There was a history of a fall from a motorcycle with some abrasions over the left arm. The child was found to have tachypnea and tachycardia and was started on noninvasive ventilation. Auscultation revealed a pansystolic murmur over the precordium. Chest X-ray revealed unilateral pulmonary edema on the right side. Echocardiography showed severe mitral regurgitation (MR) with the tear of the anterior leaflet. The child improved with diuretics and supportive care. After 3 months, he underwent surgical repair of the mitral valve. Traumatic mitral valve tear is quite rare in children. Unilateral pulmonary edema is a feature of MR with eccentric jet and is frequently misinterpreted.
Keywords: Blunt trauma, Mitral valve, Unilateral pulmonary edema.
INTRODUCTION
Cardiogenic unilateral pulmonary edema is a rare clinical condition that requires prompt identification and treatment. It is usually confined to the right upper side and is mostly caused by mitral regurgitation (MR). Here, we describe a child with traumatic MR and right-sided pulmonary edema, following blunt trauma. The child was managed conservatively initially, followed by mitral valve repair later.
CASE DESCRIPTION
A 7-year-old boy came walking to the casualty with complaints of cough and fast breathing for 1 day. There was no history of fever. Two days earlier, he fell while riding on the petrol tank of his father’s motorcycle. The child was taken to a nearby hospital, found to be normal except for abrasions over the left chest and arm, given pain relief, and then sent back home. He started having progressively worsening cough the next evening and developed breathing difficulty. Chest X-ray showed right-sided infiltrates, and he was referred to our hospital on suspicion of pneumonia (Fig. 1). In the casualty, he was able to maintain his airway and breathe spontaneously with room air saturation of 88% and had severe retractions. The blood pressure was stable, but he was tachycardic. In the background of recent trauma, bedside ultrasound screening of the abdomen and chest was performed and showed a mild right pleural effusion. Auscultation revealed decreased air entry with crepitations over the right side and a pansystolic murmur with radiation to the left axilla. Echocardiography showed a flail anterior mitral leaflet with rupture of papillary muscles (anterolateral), causing severe MR. He was shifted to the pediatric intensive care unit and started on noninvasive ventilation. Diuretics were started and the distress gradually improved. Once stable, he was started on after-load reduction with enalapril. He gradually became better and was eventually discharged. After 3 months, he underwent definitive surgery for repair of the mitral valve. Postoperatively, he is doing well and is under regular follow-up.
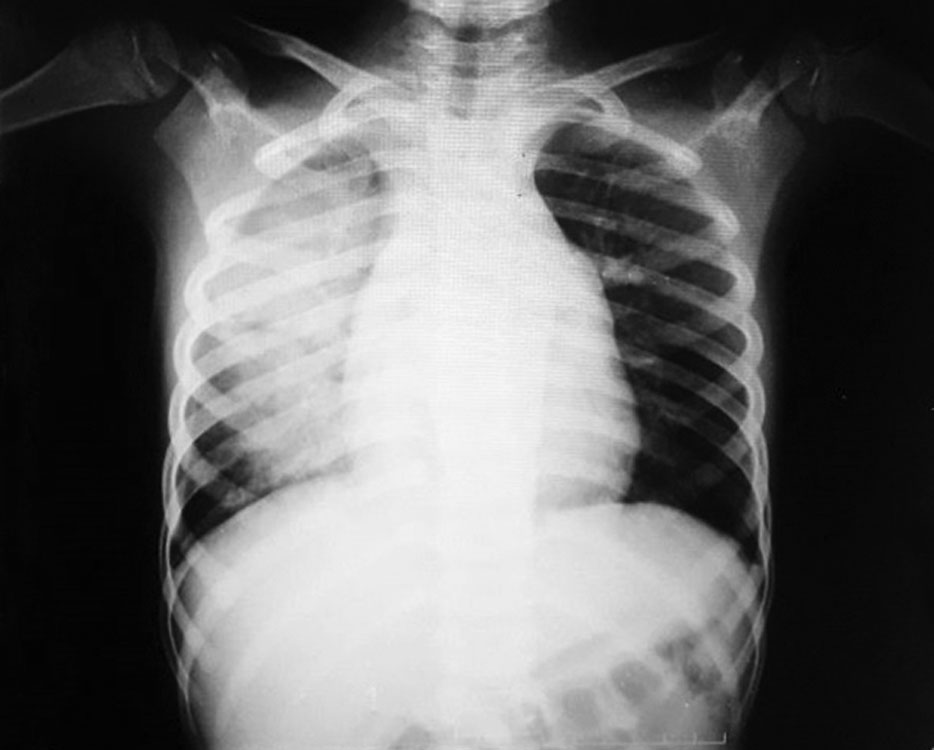
Fig. 1: Chest X-ray
HIGHLIGHTS/DISCUSSION
Cardiac injury after blunt trauma ranges from asymptomatic mild cardiac bruise to cardiac rupture.1 Cardiac injuries are frequently underreported and underevaluated in polytrauma as other obvious injuries divert the attention of the physician. Incidence of blunt cardiac injury (BCI) ranges from 20 to 79%.2
Cardiac valve injury, especially mitral, is quite rare in BCI. Parmley et al.2 and Maenza et al.3 did not report a single case of mitral valve injury and any cardiac valve injury, respectively, in their study. Ischemic MR is quite common, whereas traumatic MR has been reported rarely in the literature.4 Traumatic mitral valve rupture occurs when compression happens in the isovolumetric contraction phase when the intraventricular pressure is very high. Traumatic MR is quite rare in children. In 1991, David McCrory et al. mention a 6 years old hit by a car and developing MR, requiring prosthetic valve replacement.5 In 2001, there was a report from Turkey of the ventricular septal defect and MR following penetrating injury to the chest.6 In 2009, Eyup Hazan et al. report a 2 1/2 years old child developing mitral insufficiency due to an isolated rupture of the posterior papillary muscle following the fall of television over his chest.7
No gold standard exists for the diagnosis of BCI, and it is difficult to predict the patients vulnerable to develop complications. BCI was hence classified as: (1) BCI with cardiac-free wall rupture, (2) BCI with cardiac septal rupture, (3) BCI with coronary artery injury, (4) BCI with cardiac failure, (5) BCI with complex arrhythmia, and (6) BCI with minor ECG or cardiac enzyme abnormalities.1
Forteleoni et al. in 2019 conducted a systematic review of 192 patients with traumatic mitral valve regurgitation following blunt trauma.8 Transesophageal echocardiography (TEE) is a better choice to detect anatomic defects causing mitral valve dysfunction compared to transthoracic echocardiography (TTE) as the latter may be difficult due to poor window and high thoracic impedance in relation to pulmonary edema following blunt chest trauma.9
Mitral valve injury can involve the valve leaflet, papillary muscle, or the chordae tendineae. Posterior mitral leaflet has a weaker chordae tendineae and is more prone to rupture than the anterior leaflet.10 Papillary muscles are supplied by long epicardial vessels, and hence, injury to these vessels leads to gradual necrosis of the chordae and delayed rupture of the valve. Unilateral pulmonary edema is rare in pediatrics. Unilateral infiltrates in children usually represent pneumonia or atelectasis. The clinician may pursue these diagnoses without realizing that other disease states and procedures in pediatrics predispose to unilateral pulmonary edema. Steven M Audenaurt describes three children with unilateral pulmonary edema as follows:
- A 20-day-old baby with coarctation of aorta and right-sided pulmonary edema. In this patient, this pattern of perfusion has been attributed to obstruction of the left mainstem bronchus by an enlarged left atrium. This led to alveolar hypoxia and hypoxic pulmonary vasoconstriction. Flow is, therefore, redirected from the left lung to the right, where vascularity increases, and pulmonary edema may result.
- A child with chronic renal failure and congestive cardiac failure and left-sided pulmonary edema. In this child, left-sided unilateral pulmonary edema occurred due to congestive failure.
- A child with lymphoma with reexpansion pulmonary edema following a large volume pleurocentesis.11 Unilateral pulmonary infiltrates and even localized infiltrates thus may represent pulmonary edema from any number of causes and should not be assumed to be of infectious etiology.11 Even neurogenic pulmonary edema can be seen as a unilateral phenomenon.12 It is difficult to differentiate the etiology clinically or radiologically of such findings. The absence of fever and history of trauma can give us an indication for noninfectious etiology as in our child. The presence of a new-onset murmur in a previously normal child can also point us toward infiltrate versus fluid in the lung.
Mitral valve regurgitation is understood to cause pulmonary edema as a result of increased intravascular hydrostatic pressure. Predominantly right upper lobe edema may be caused by a directed regurgitant jet with resultant local increases in hydrostatic pressure. Schnyder and coworkers reported a 9% prevalence of predominantly right upper lobe pulmonary edema in cases of severe mitral valve regurgitation.13 In 1982, Miyatake et al.14 showed that the direction of the regurgitant jet caused by flail mitral valve leaflets varies depending on the leaflet involved. Roach’s group15 later reported that the jet of regurgitant flow in a patient with a flail posterior valve leaflet is directed specifically toward the right pulmonary vein. But in our child, it was the flail anterior mitral leaflet and the entire right lung was involved.
CONCLUSION
BCI, particularly valvular injuries, is rare in children. They are often not recognized early as other obvious injuries divert the attention of the clinician. Unilateral pulmonary edema, particularly of the right side, is a feature of MR that is often confused radiologically with infectious etiology. The presence of a new-onset murmur with unilateral lung infiltrates can be present in cardiogenic pulmonary edema due to acute MR following blunt chest trauma.
ORCID
Satarupa Mukherjee https://orcid.org/0000-0002-4526-8620
K Ravikumar https://orcid.org/0000-0003-0227-9423
Sudeep K Kapalavai https://orcid.org/0000-0001-6818-4158
Bala Ramachandran https://orcid.org/0000-0003-2153-0126
REFERENCES
1. Mattox KL, Flint LM, Carrico CJ, Grover F, Meredith J, Morris J, et al. Blunt cardiac injury. J Trauma Inj Inf Crit Care 1992;33(5):649–650. DOI: 10.1097/00005373-199211000-00001.
2. Parmley LF, Mattingly TW. Non-penetrating traumatic injury of the heart. Circulation 1958;18:371–396. DOI: 10.1161/01.cir.18.3.371.
3. Maenza RL, Seaberg D, D’Amico F. A meta-analysis of blunt cardiac trauma: ending myocardial confusion. Am J Emerg Med 1996;14(3):237–241. DOI: 10.1016/s0735-6757(96)90165-5.
4. Pasquier M, Sierro C, Yersin B, Delay D, Carron P-N. Traumatic mitral valve injury after blunt chest trauma: a case report and review of the literature. J Trauma Inj Inf Crit Care 2010;6(1):243–246. DOI: 10.1097/ta.0b013e3181bb881e.
5. McCrory D, Craig B, O’Kane H. Traumatic mitral valve rupture in a child. Ann Thorac Surg 1991;51(5):821–822. DOI: 10.1016/0003-4975(91)90138-g.
6. Golbasi Z, Cicek D, Ucar O, Kaya D, Keles T, Cicekcioglu H, Aydogdu S. Traumatic ventricular septal defect and mitral insufficiency after a Kebab’s Shish wound to the chest. Eur J Echocardiogr 2001;2:203–204. DOI: 10.1053/euje.2001.0074.
7. Hazan E, Guzeloglu M, Sariosmanoglu N, Ugurlu B, Keskin V, Unal N. Repair of isolated mitral papillary muscle rupture consequent to blunt trauma in a small child. Tex Heart Inst J 2009;36(3):252–254.
8. Forteleoni A, Montereggi F, Sanna GD, Portoghese M, Parodi G. Traumatic mitral valve regurgitation: a case report and state-of-the-art review. J Cardiovasc Med 2019;20(10):709–717. DOI: 10.2459/jcm.0000000000000809.
9. Karalis DG, Victor MF, Davis GA, McAllister MPJ, Covalesky VA, Ross JJ, et al. The role of echocardiography in blunt chest trauma: a transthoracic and transesophageal echocardiographic study. J Trauma 1994;36:53–58. DOI: 10.1097/00005373-199401000-00008.
10. Selzer A, Kelly JJ, Vannitamby M, Walker P, Gerbode F, Kerth WJ. The syndrome of mitral insufficiency due to isolated rupture of the chordae tendineae. Am J Med 1967;43(6):822–836. DOI: 10.1016/0002-9343(67)90241-0.
11. Audenaert SM. Unilateral pulmonary edema in children. Clin Pediat 2016;32:363–365. DOI: 10.1177/000992289303200609.
12. Goff NW, Weese WC. A case of unilateral neurogenic pulmonary edema. Ariz Med 1981;38:832–833.
13. Schnyder PA, Sarraj AM, Duvoisin BE, Kapenberger L, Landry MJ. Pulmonary edema associated with mitral regurgitation: prevalence of predominant involvement of the right upper lobe. AJR Am J Roentgenol 1993;161:33–36. DOI: 10.2214/ajr.161.1.8517316.
14. Miyatake K, Nimura Y, Sakakibara H, Kinoshita N, Okamoto M, Nagata S, et al. Localisation and direction of mitral regurgitant flow in mitral orifice studied with combined use of ultrasonic pulsed Doppler technique and two dimensional echocardiography. Br Heart J 1982:48:449–458. DOI: 10.1136/hrt.48.5.449.
15. Roach JM, Stajduhar KC, Torrington KG. Right upper lobe pulmonary edema caused by acute mitral regurgitation. Diagnosis by transesophageal echocardiography. Chest 1993;103:1286–1288. DOI: 10.1378/chest.103.4.1286.
________________________
© The Author(s). 2021 Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (https://creativecommons.org/licenses/by-nc/4.0/), which permits unrestricted use, distribution, and non-commercial reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated.